Can DVT Go Away Without Treatment?
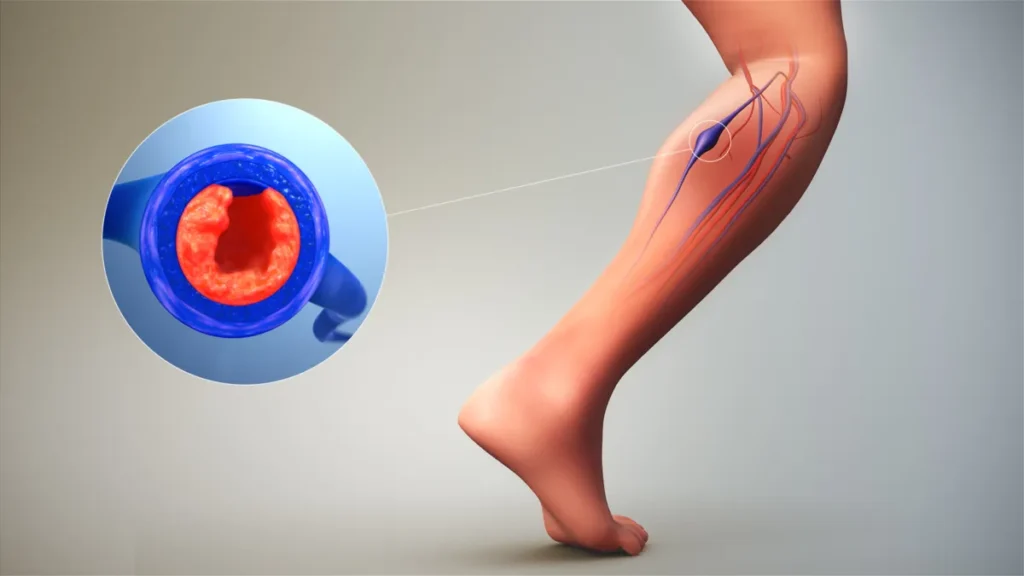
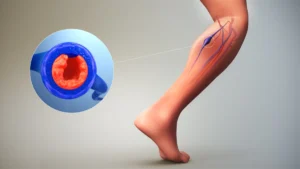
Understanding Deep Vein Thrombosis
Deep vein thrombosis (DVT) occurs when a blood clot forms in a deep vein, most commonly in the legs. This serious condition affects approximately 900,000 Americans each year and requires proper understanding to recognize risks and symptoms early.
Causes and Risk Factors
DVT develops when blood flow becomes sluggish or when the inner lining of a vein is damaged. Several factors can increase the risk of developing this condition. Prolonged immobility, such as during long flights or hospital stays, significantly reduces blood circulation in the legs.
Surgery, especially orthopedic procedures, can damage blood vessels and trigger clot formation. Certain medical conditions like cancer, heart failure, and inflammatory bowel disease also elevate DVT risk.
Genetic factors play a role as well, with inherited blood clotting disorders making some individuals more susceptible to DVT or PE. Age is another important factor, with people over 60 facing higher risks.
Other common risk factors include:
- Obesity
- Smoking
- Pregnancy and postpartum period
- Hormone therapy
- Previous history of DVT
Symptoms of DVT
DVT symptoms vary in intensity and some cases may be asymptomatic. The most common sign is swelling in one leg, particularly the calf area. This swelling often develops gradually over hours or days in the lower leg.
Pain or tenderness in the affected area frequently accompanies swelling. This discomfort typically feels like a cramp or soreness that worsens when standing or walking.
Skin discoloration around the affected area is another warning sign. The skin may appear reddish or bluish compared to the other leg, particularly around the location of the clot.
Some patients report a feeling of warmth in the affected area. In severe cases, visible surface veins may become more prominent.
It’s important to note that approximately 50% of DVT cases show no symptoms, making awareness of risk factors crucial for prevention.
DVT and Pulmonary Embolism
The most dangerous complication of DVT is pulmonary embolism (PE), a potentially life-threatening condition. PE occurs when a blood clot breaks free from a vein wall and travels through the bloodstream to the lungs.
Once in the lungs, the clot can block blood flow to vital lung tissue. This blockage prevents normal oxygen exchange, which can be fatal if not treated promptly.
Symptoms of PE include sudden shortness of breath, chest pain that worsens with deep breathing, rapid heart rate, and sometimes coughing up blood. These symptoms require immediate medical attention.
The risk of developing PE from untreated DVT is significant, with approximately 30% of untreated DVT cases leading to pulmonary embolism. Early detection and proper management of DVT are essential to prevent this serious complication.
Treatment Options for DVT
Deep vein thrombosis (DVT) requires prompt medical attention to prevent serious complications such as pulmonary embolism (PE). Several effective treatments exist, ranging from medication-based approaches to mechanical interventions depending on the severity and location of the blood clot.
Anticoagulant Medications
Anticoagulants, commonly known as blood thinners, are the primary treatment for DVT. These medications prevent existing clots from growing larger and reduce the risk of new clot formation.
Common anticoagulants include:
- Warfarin (Coumadin) – requires regular blood tests to monitor effectiveness in preventing DVT and PE.
- Direct oral anticoagulants (DOACs) – including rivaroxaban, apixaban, and dabigatran
- Heparin – often used initially in hospital settings before transitioning to oral options
Treatment typically continues for 3-6 months, though some patients require longer therapy based on risk factors. The dosage and duration depend on the cause of DVT and whether it’s a first-time or recurring event.
Blood thinners carry some risk of bleeding complications, so patients should be monitored regularly by healthcare providers. At facilities like Big Apple Medical Care in Brooklyn, specialists create personalized treatment plans to balance clot prevention with bleeding risk.
Compression Stockings and Management
Compression stockings play a crucial supportive role in DVT treatment and prevention. These specially designed garments apply graduated pressure to the legs, promoting blood flow and reducing swelling.
Benefits of compression therapy:
- Decreases pain and swelling in the affected limb
- Helps prevent post-thrombotic syndrome, a long-term complication of DVT
- Reduces the risk of recurrent venous thromboembolism
Patients should wear compression stockings during the day and remove them at night. The recommended pressure level varies based on individual needs, typically ranging from 20-30 mmHg or 30-40 mmHg.
Physical activity is also encouraged once initial treatment begins. Walking regularly helps improve circulation and speeds recovery. However, patients should avoid strenuous activities until cleared by their doctor.
Surgical Interventions
In severe cases of DVT, particularly when blood clots are large or causing significant symptoms, surgical or catheter-directed interventions may be necessary.
Advanced treatment options for DVT and PE include:
- Catheter-directed thrombolysis: Delivering clot-dissolving medications directly to the thrombus
- Thrombectomy: Surgical removal of the blood clot
- Inferior vena cava (IVC) filter: A device implanted to catch blood clots before they reach the lungs
These procedures are typically reserved for patients with massive clots, those who cannot take anticoagulants, or when medication alone isn’t effective. At specialized vascular centers, including those affiliated with practitioners at 7322 5th Ave in Brooklyn (718-333-5120), interventional radiologists perform these procedures with minimally invasive techniques.
Recovery time varies based on the intervention performed. Patients require close follow-up care to monitor healing and prevent recurrence of venous thromboembolism.
Natural Progression and Complications
Deep vein thrombosis (DVT) follows a variable course when left untreated, with outcomes ranging from spontaneous resolution to life-threatening complications. Understanding this natural progression is crucial for patients weighing treatment options.
Potential for Spontaneous Resolution
Some cases of DVT may resolve without medical intervention. The body’s natural clot-dissolving system, called fibrinolysis, can gradually break down blood clots. Studies suggest approximately 20% of calf DVTs may dissolve spontaneously within days to weeks.
However, this natural resolution is unpredictable and depends on clot size, location, and individual factors. Larger proximal clots in the thigh or pelvis are less likely to resolve on their own compared to smaller distal clots in the calf.
The risk during this “wait-and-see” approach remains significant. Without treatment, approximately 50% of calf DVTs will extend proximally, increasing complication risks dramatically, potentially leading to another clot.
Healthcare providers at specialized centers like Big Apple Medical Care emphasize that hoping for spontaneous resolution without medical monitoring is dangerous. Blood thinners remain the standard of care for most DVT cases.
Long-Term Complications
Untreated DVT can lead to several serious long-term complications affecting quality of life and survival rates. The most immediate risk is pulmonary embolism (PE), occurring when part of the clot breaks off and travels to the lungs.
PE happens in approximately 50% of untreated proximal DVT cases and carries a 30% mortality rate if left untreated. Even when not immediately fatal, recurrent clots may develop in about 30% of untreated patients within 5 years, leading to another DVT.
Chronic thromboembolic pulmonary hypertension (CTEPH) can develop in 2-4% of PE cases. This condition occurs when clots in pulmonary arteries don’t dissolve, causing increased pressure in these vessels.
Damage to venous valves is virtually inevitable with untreated DVT, leading to chronic venous insufficiency. The inferior vena cava may also be compromised in extensive clotting, causing widespread circulatory issues.
Post-Thrombotic Syndrome
Post-thrombotic syndrome (PTS) represents the most common long-term complication of untreated or under-treated DVT. This chronic condition develops in 20-50% of DVT patients, typically within 1-2 years after the initial clot.
PTS occurs due to damage to venous valves and persistent venous hypertension. Symptoms of DVT include:
- Chronic leg pain and heaviness
- Swelling that worsens with activity
- Skin discoloration and thickening
- Venous ulcers (in severe cases)
The severity of PTS correlates with the extent and location of the initial DVT. Proximal clots carry higher risk than distal ones. Once established, PTS has no cure and management focuses on compression therapy and symptom control.
Prevention through prompt DVT treatment is far more effective than treating established PTS. Without proper anticoagulation, the risk of developing moderate to severe post-thrombotic syndrome (PTS) in people with DVT increases by approximately 250%.
Prevention and Prognosis of DVT
Preventing Deep Vein Thrombosis (DVT) is crucial, especially for individuals with known risk factors. Regular movement is one of the most effective preventive measures, as prolonged immobility significantly increases clot formation risk.
Key DVT Prevention Strategies:
- Stay hydrated, especially during long flights or car trips
- Avoid sitting or standing for extended periods
- Exercise regularly to maintain healthy circulation
- Wear compression stockings if recommended by a healthcare provider
- Maintain a healthy weight
For those with higher risk profiles, physicians may prescribe blood thinners (anticoagulants) as a preventive measure. These medications help reduce blood’s clotting ability, decreasing the likelihood of new clots forming.
Individuals with prior DVT history face approximately 30% risk of recurrence within 10 years. This risk is highest within the first year after the initial event.
The prognosis for DVT varies based on clot size, location, and prompt treatment. With proper medical intervention, most DVT cases resolve without complications. However, untreated DVT can lead to serious consequences.
DVT Risk Factors to Monitor:
- Recent surgery or hospitalization
- Cancer diagnosis
- Pregnancy or hormone therapy
- Family history of blood clots
- Prolonged immobility
- Age (risk increases after 60)
Early diagnosis significantly improves outcomes. Medical facilities like specialized vascular clinics offer comprehensive care for both prevention and treatment of existing clots, helping prevent their growth and expansion.
Frequently Asked Questions
Deep vein thrombosis generates many questions from patients concerned about symptoms, detection, and outcomes. These questions often focus on early warning signs, detection timeframes, and potential consequences if left untreated.
What are the symptoms of a DVT in the early stages?
Early DVT symptoms include swelling, pain, tenderness, warmth, and redness in the affected area, typically the leg.
How long might a person have a DVT before being aware of it?
A person may have DVT for days or even weeks before experiencing noticeable symptoms, as some clots develop silently.
What is the life expectancy following a diagnosis of DVT?
Life expectancy after DVT diagnosis is generally normal with proper treatment, though patients have a higher risk of recurrence.
At what rate can a blood clot travel from the leg to the lungs?
A blood clot can travel from the leg to the lungs within seconds to minutes once it breaks free.
What is the accuracy of a calf squeeze test in diagnosing DVT?
The calf squeeze test (Homans’ sign) has limited accuracy for DVT diagnosis, with sensitivity around 10-54% and specificity of 39-89%.
What are the typical treatment options for deep vein thrombosis?
Typical DVT treatments include anticoagulants, compression stockings, and in severe cases, thrombolytics or surgical interventions.